Introduction
Life care planning has emerged as an essential framework for addressing the long-term needs of individuals with catastrophic injuries, chronic health conditions, and disabilities (Broyles et al., 2016; Deutsch & Raffa, 1981; Deutsch & Sawyer, 2002; International Academy of Life Care Planners, 2022; Katz, 2019; Reid et al., 2025; Rutherford Owen, 2025). As a systematic and individualized process, life care planning provides a comprehensive projection of future medical care, personal assistance, equipment needs, therapeutic services, and support systems, all of which are designed to optimize health outcomes, enhance quality of life, and promote community integration (International Association of Rehabilitation Professionals, 2025). Moreover, life care plans assist in securing appropriate support, guiding legal decisions, facilitating insurance and benefits determinations, and informing long-term financial planning for individuals with disabilities and complex medical conditions (Weed & Berens, 2018). Life care plans have become foundational documents in litigation (Caragonne & Male, 2003; Deutsch & Raffa, 1981; IMS Legal Strategies, 2025; Mills, 2024), rehabilitation (Berens & Weed, 2010; Johnson, 2024; Reid & Riddick-Grisham, 2015; Skelton et al., 2022) and disability management settings (Bagnell & Moberg-Wolff, 2024; Crowley & Huber, 2024; Rutherford Owen et al., 2024; Weed & Berens, 2018), yet despite the extensive research and evolution of best practices in this field, one critical domain remains consistently overlooked: disaster preparedness.
The increasing frequency and severity of natural and human-made disasters present substantial risks to individuals with complex care needs (Centers for Disease Control and Prevention, 2024; Nishioka, 2024). Disasters disrupt access to medical care, compromise the availability of assistive technology, undermine accessible transportation, and create significant barriers to evacuation and sheltering, thereby compounding the vulnerability of these populations (Kouadio et al., 2012; Lamberti-Castronuovo et al., 2022; World Health Organization, 2025). For individuals whose health, safety, and functional independence rely on specialized care, equipment, and environmental modifications, these disruptions can have devastating and even life-threatening consequences (Lindsay et al., 2023; Lindsay & Hsu, 2024; Subramaniam & Villeneuve, 2020; Williams, 2025). Yet, despite the known risks, disaster preparedness remains largely absent from formal conversations and research focused on life care planning across the lifespan.
This article addresses this notable absence by examining the intersection of life care planning and disaster preparedness, identifying critical research gaps, and providing evidence-informed recommendations for incorporating emergency planning as a standard, essential component of life care plans.
Methods
A structured literature review was conducted to examine the extent to which disaster preparedness is addressed within life care planning frameworks for individuals with disabilities, chronic health conditions, and complex care needs. The review aimed to identify existing research, practice guidelines, and professional discourse related to the integration of emergency planning in life care plans across the lifespan.
The search included peer-reviewed journal articles, professional guidelines, textbooks, and additional sources such as government documents, organizational reports, and conference materials published between 2000 and 2025, with an emphasis on materials published within the last 10 years to ensure contemporary relevance. The following electronic databases were searched: EMBASE, PubMed, PsycINFO, Scopus, CINAHL, and Google Scholar. Additionally, relevant professional organizations’ websites, including the Center for Disease Control (CDC), Office of Disability Integration and Coordination (ODIC)-FEMA, American Association on Intellectual and Developmental Disabilities (AAIDD), International Academy of Life Care Planners (IALCP), International Association of Rehabilitation Professionals (IARP), Foundation for Life Care Planning Research (presently Foundation for Life Care Planning and Rehabilitation Research), and National Council on Disability, were examined for policy documents, reports, and practice guidelines.
Search terms were developed using combinations of the following keywords and Boolean operators (AND, OR): Life Care Planning, Disaster Preparedness, Emergency Planning, Disability Management, Rehabilitation, Continuity of Care, Vulnerable Populations, Catastrophic Injury, and Long-Term Care. Reference lists of relevant articles were also manually reviewed to capture additional sources not identified through electronic searches. Inclusion criteria were as follows: (1) peer-reviewed journal articles, professional reports, book chapters, or authoritative grey literature; (2) publications addressing life care planning, disaster preparedness, or their intersection; (3) materials focused on individuals with disabilities, chronic conditions, or complex care needs; and (4) English-language publications. Exclusion criteria included: (1) articles not addressing life care planning or disaster preparedness; (2) publications focused solely on emergency response unrelated to disability or long-term care; (3) non-English-language materials; and (4) opinion pieces lacking an empirical or practice-based foundation.
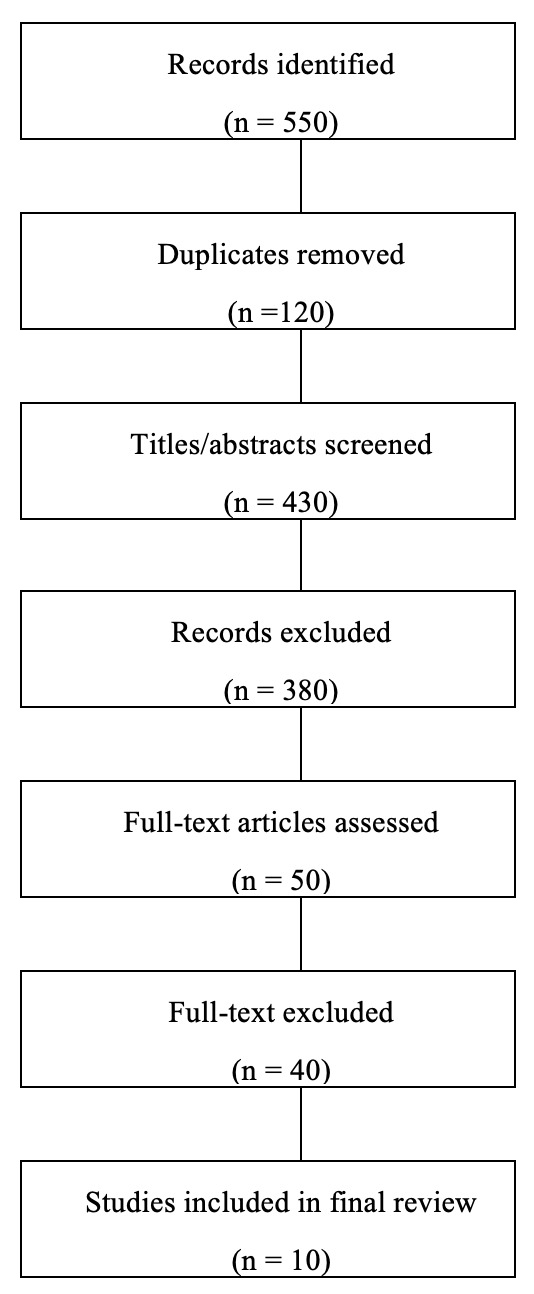
The search process identified 550 publications, and duplicates were removed. After removing 120 duplicates, 430 titles and abstracts were screened for relevance. Of these, 380 were excluded as they did not address life care planning, disaster preparedness, or disability-related contexts. The remaining 50 full-text articles were assessed for eligibility. Following full-text review based on the inclusion and exclusion criteria, 10 publications were deemed suitable for inclusion in the final review. Data from these sources were extracted, including publication type, population focus, relevance to life care planning and disaster preparedness, key findings, and identified research and practice gaps.
Thematic analysis was employed to synthesize the findings. Following Braun and Clarke’s (2006) six-phase framework for thematic analysis; an inductive approach was utilized to identify patterns and concepts within the extracted data. This process involved an initial phase of familiarization, during which the selected publications were read and re-read to ensure a comprehensive understanding of the content. Subsequently, open coding was conducted to identify recurring ideas, language, and content relevant to life care planning, disaster preparedness, and disability management. Codes were then reviewed, refined, and grouped into potential themes based on conceptual similarities and their relevance to the research question. To enhance rigor and reduce bias, an independent reviewer was consulted to examine the emerging codes and themes, ensuring coherence, consistency, and alignment with the research objectives. The themes were further defined and named, ensuring that each captured a distinct aspect of the phenomenon under investigation.
Three primary themes emerged from the analysis, providing a conceptual framework for understanding the intersection of disaster preparedness and life care planning. These themes are: (1) heightened vulnerability in Disaster Situations for Individuals with Complex Care Needs, which captures the disproportionate exposure to risk experienced by individuals with disabilities and chronic conditions during disasters; (2) systemic gaps in Life Care Planning Practices, which reflects the widespread absence of standardized approaches to incorporating disaster preparedness within life care plans; and (3) the imperative for integrated disaster preparedness in life care planning, which emphasizes the ethical, practical, and clinical justifications for embedding emergency planning into life care plans as a core component of comprehensive care. These themes inform the structure, interpretation, and recommendations presented in this article.
Heightened Vulnerability in Disaster Situations for Individuals with Disabilities and Complex Care Needs
A substantial body of literature underscores the disproportionate impact of disasters on individuals with disabilities and complex health conditions. Research from the National Council on Disability (2023), and The United Nations Office for Disaster Risk Reduction (2023), emphasizes individuals with disabilities face greater challenges during disasters, including limited access to evacuation, healthcare, and shelter. Likewise, Urban Institute (2025) documented how poorly designed emergency management systems often exclude disability-specific needs, resulting in increased morbidity and mortality.
The COVID-19 pandemic highlighted these vulnerabilities on a global scale, with disruptions in home care, medical supplies, and access to essential services disproportionately affecting individuals with disabilities (Boyle et al., 2022). Other disasters, such as Hurricanes Katrina, Ian, and Helene, revealed systemic failures in protecting individuals with disabilities during large-scale emergencies (Stough & Kelman, 2018). More recently, the Los Angeles wildfires, including the Eaton and Palisades fires that destroyed thousands of homes and displaced over 200,000 residents, again underscored this persistent oversight (AP News, 2025). Recent findings from the UNDRR Global Survey (2023) confirm that individuals with disabilities remain significantly underrepresented in community disaster preparedness efforts. These persistent gaps underscore the critical need for personalized and disability-inclusive emergency planning. Yet, formal processes continue to overlook the integration of disaster preparedness as a standard component in overall life care planning.
Systemic Gaps in Life Care Planning Practices
Life care planning is intended to anticipate and address the full spectrum of future care needs for individuals with catastrophic injuries, disabilities, or chronic health conditions (Weed & Berens, 2018; IALCP, 2022). However, as the frequency and severity of natural disasters and public health emergencies continue to escalate globally (Centers for Disease Control and Prevention, 2024; Nishioka, 2024; World Health Organization, 2025), there remains a troubling disconnect between the known risks faced by individuals with disabilities during emergencies and the contents of formal life care plans.
A systematic review of peer-reviewed literature, professional practice guidelines, and published life care plan examples revealed a consistent omission of structured, evidence-informed approaches to disaster preparedness within life care planning. Although some plans may make passing reference to backup power for medical equipment or general home safety measures (Kailes & Enders, 2007; Lindsay & Hsu, 2024; Williams, 2025), comprehensive strategies for ensuring client safety, care continuity, and accessibility in the context of emergencies (i.e. wildfires, hurricanes, floods, and public health crises) are rarely, if ever, included in a standardized manner. Furthermore, the review identified no peer-reviewed studies that directly examine how disaster preparedness considerations could or should be operationalized within life care planning frameworks. This absence leaves life care planners without clear protocols, assessment tools, or evidence-based guidelines to inform this critical aspect of future care planning. The lack of research and professional consensus also limits opportunities for interdisciplinary collaboration between life care planners, emergency management professionals, disability advocates, and public health authorities. This systemic gap has significant real-world consequences; when life care plans fail to account for disaster preparedness, they fall short of their fundamental purpose which is to ensure continuity of care, safeguard quality of life, and mitigate preventable harm for individuals with complex care needs.
Given the clear vulnerabilities and increasing disaster risks, there is a pressing need for research, policy development, and professional training to close this gap. It is essential that life care plans be expanded to incorporate practical, individualized disaster preparedness strategies as a standard element, ensuring that individuals with disabilities and complex care needs are equipped not only for everyday life but also for the challenges posed by emergencies and unforeseen events.
Imperative for Integrated Disaster Preparedness in Life Care Planning
Incorporating disaster preparedness into life care planning is no longer optional but an essential, ethical, and practical requirement. As disasters become more frequent and severe, the failure to proactively address emergency scenarios leaves individuals with disabilities and complex care needs at significant risk. Life care plans, designed to anticipate long-term medical, functional, and support requirements, must also account for the unpredictable challenges posed by natural disasters, public health emergencies, and infrastructure failures.
The consequences of excluding disaster preparedness from life care plans are well-documented. Disruptions to power, transportation, and healthcare systems can leave individuals with disabilities without access to essential medical equipment, medications, or assistive technologies, which, when lost, can sharply increase the risk of hospitalization or even death during emergencies. Recent data shows that medically relevant power outages (lasting 8 or more hours) frequently coincide with hurricanes and other extreme weather events, disproportionately affecting regions with high reliance on durable medical equipment (DME) (Li et al., 2023). Additionally, guidance from disability advocacy groups highlights emergency power planning as a critical risk mitigation strategy for individuals reliant on electrified assistive devices such as ventilators, oxygen concentrators, and power wheelchairs (ADA National Network, 2023). By integrating disaster planning into life care plans, professionals ensure not only continuity of care but also reduce the likelihood of medical complications, psychological distress, and avoidable health crises when emergencies occur (Boyle et al., 2022).
The financial implications of unplanned disasters are also significant. The replacement of expensive medical equipment, home modifications, or assistive devices following a disaster can create substantial financial burdens for individuals and families. Thoughtful, individualized preparedness strategies such as identifying funding sources, securing insurance coverage, and outlining replacement protocols can help mitigate these costs and promote financial stability. Evidence shows that investing in disaster risk reduction yields high returns with each dollar spent saving an estimated three to five dollars in potential losses, including medical and property costs (World Bank, 2021).
Perhaps most critically, integrating disaster preparedness into life care planning reflects the legal and ethical obligations of life care planners to protect the dignity, autonomy, and safety of those they serve. Emergencies disproportionately threaten the rights and well-being of individuals with disabilities, often amplifying barriers to accessible shelter, evacuation, and continuity of support services. By proactively addressing these risks, life care planners fulfill their professional responsibility to promote equitable, person-centered care, even under the most challenging circumstances (Rutherford Owen et al., 2024; Weed & Berens, 2018).
Ultimately, disaster preparedness cannot be viewed as a separate or secondary consideration. It must be woven into the fabric of life care planning as a standard, individualized component ensuring that those with disabilities and complex care needs are equipped not only for daily life, but for the uncertainties that emergencies inevitably present.
Practical Recommendations for Life Care Planners
Life care planners are uniquely positioned to strengthen the safety, autonomy, and well-being of individuals with disabilities by incorporating practical, individualized disaster preparedness strategies into their work. Building on their expertise in comprehensive care planning, life care planners can proactively support clients and families in navigating the risks associated with emergencies by considering the following approaches:
-
Integrate Disaster Risk Assessments: Include an individualized evaluation of disaster vulnerability as part of the life care planning process, ensuring that environmental, functional, and health-related risks are identified early.
-
Foster Interdisciplinary Collaboration: Engage with emergency management professionals, disability advocacy groups, and community organizations to stay informed and ensure that clients benefit from inclusive preparedness initiatives.
-
Plan for Equipment Continuity: Recommend reliable backup power solutions for life-sustaining medical equipment and assistive technology, tailored to each evaluees needs and living environment.
-
Facilitate Safe Evacuation Options: Identify accessible evacuation routes, transportation resources, and shelter options that meet the specific mobility, communication, and support requirements of the individual.
-
Prepare for Financial Resilience: Document replacement costs for critical equipment and home modifications, supporting insurance claims and financial planning in the aftermath of a disaster.
-
Empower Through Resources: Provide evaluees and families with trusted, accessible resources such as FEMA’s Ready.gov materials and disability-focused emergency planning guides.
-
Promote Ongoing Preparedness Conversations: Engage evaluees and their support networks in regular, collaborative discussions about evolving risks, emerging preparedness strategies, and personalized action plans.
-
Support Mental Health Preparedness: Recognize the psychological impacts of disasters and include strategies to maintain continuity of mental health care and emotional well-being during and after emergencies.
By adopting these approaches, life care planners can support evaluees not only plan for daily life but prepare them for the unexpected while ultimately promoting safety, dignity, and resilience.
Conclusion
The intersection of life care planning and disaster preparedness represents a significant, yet overlooked, area of practice and research. As the frequency and severity of disasters grow, individuals with disabilities and chronic health conditions remain disproportionately at risk when continuity of care, access to medical equipment, and supportive services are disrupted. Life care planners are uniquely positioned to close this gap by embedding individualized preparedness strategies directly into their plans.
Life care plans can be enhanced by focusing more intentionally on evacuation options, continuity of essential equipment, financial preparedness, and psychosocial support. Developing these elements in collaboration with emergency management professionals, healthcare providers, and disability advocates ensures that plans are not only practical but also inclusive of the diverse needs of those they serve. With this approach, life care plans move beyond static documents to become adaptable tools that strengthen resilience, equity, and long-term safety. Ultimately, incorporating disaster preparedness should not be viewed as an optional addition but as a core responsibility of the profession. By integrating emergency planning as a standard component, life care planners can better safeguard continuity of care, protect quality of life, and reduce preventable harm for individuals who are most vulnerable when disasters occur.